Lost in the overload of coronavirus news was a significant medical discovery that was announced on the nature Communications website in July 2020. The article entitled "Non-invasive early detection of cancer four years before conventional diagnosis using a blood test" by Xingdong Chen et al would appear to be a very significant development for all of us, particularly those, who like me, are predisposed to certain types of cancer.
Those of us that have had family members and friends die from late stage cancers that were detected at a stage where effective treatments were not available may now have some hope given that this research suggests that early detection is possible. As we know, survival rates from most cancers improves significantly when that cancer is identified at early stages, offering the options of surgical removal or treatment with milder forms of chemotherapy. The average five-year survival rate when cancer is discovered at an early stage is 91 percent, dropping to only 26 percent when cancers are discovered in late stage. While there are some screening measures available for a few types of cancers, some involve invasive procedures (think colonoscopy) and some are not terribly effective.
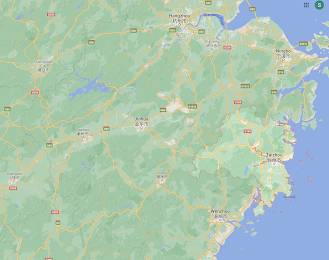
As background, the Taizhou Longitudinal Study began in July 2007 with the goal of recruiting at least 100,000 people in the city of Taizhou in China for a health study, following the participants for at least 40 years. Here is a map showing the location of Taizhou which is located at the mouth of the Jiaojiang River along the shore of the East China Sea:
The Taizhou study was designed to explore the roles of many important environmental factors, particularly those related to the economic transformation in China, in common chronic diseases both genetic and non genetic. DNA was extracted from participants as well as buccal mucosal cells and blood specimens. Each participant was subjected to an interviewer-administered questionnaire and their anthropometric measurements were taken (height, weigh etcetera). Only healthy subjects ranging in age from 30 to 80 years were eligible to participate in the study. A follow-up survey was conducted every three years to obtain information on the occcurance of diseases as well as information on lifestyle exposures. A total of 123,115 individuals were voluntarily recruited and, at this point, the average follow-up time is 8.1 years.
In Taizhou, the incidence of digestive cancers is quite high with esophageal, gastric and liver cancers being quite common in comparison to the rest of China. According to statistics from 2010, the cancer mortality rate for residents of Taizhou was 154.05 per 100,000 person-years, nearly twice the mean incidence rate for all of China.
In total, 1.6 million blood samples were taken from the volunteers, samples were then centrifuged and plasma was separated out and placed into long-term storage at -80 degrees Celsius or below. The subjects were then monitored for the occurrence of cancer through the use of annual health checks.
With this background, let’s now look at the study. The researchers in the aforementioned study analyzed DNA samples isolated from collected samples of both fresh cancer and healthy tissue using their PanSeer assay which detects methylation patterns in DNA, a biological process that occurs when a methyl (CH3) group is added to DNA, modifying the function of the genes and affecting gene expression. Past studies have shown that abnormal methylation can signal various types of cancer. The PanSeer test isolates DNA from the blood sample and measures DNA methylation at 477 regions that are cancer-specific. A machined-learning algorithm then compiles the findings into a score which indicates a person's likelihood of developing one of five specific types of cancer.
By the end of 2015, 575 initially healthy and asymptomatic subjects were diagnosed with one of five common cancer types; stomach, esophagus, colorectal, lung and liver within 4 years of the initial blood sample. Researchers tested blood samples from 191 of these cancer subjects, paired with the same number healthy individuals and found that they were able to detect cancer up to four years before symptoms appeared with a 90 percent accuracy rate and a 5 percent false-positive rate. Sensitivity ranged from 91 percent detection in esophageal cancer to 100 percent detection in liver cancer.
This research could ultimately lead to the development of a commercially available test which can be used to screen for cancer. Given that a comparatively small volume of DNA is needed from only a single tube of blood is necessary, PanSeer has the potential to be a front-line, inexpensive cancer screening tool. Once PanSeer detects the potential presence of cancer, further pathological examination could confirm its presence.
The only "fly in the ointment" could be Big Pharma. If this method becomes commercially available and is able to detect cancers before they become life-threatening, how will Big Pharma be able to sell their massively overpriced cancer drugs to desperate patients who are willing to pay just about any amount to prolong their lives?
Click HERE to read more from this author.
You can publish this article on your website as long as you provide a link back to this page.

Be the first to comment