One thing that has become readily apparent during the age of COVID is the controversial use of universal masking. Science regarding the use of masks to protect us against the SARS-CoV-2 virus and other similar viruses is extremely divisive with each side of the debate having its own "axe to grind". That said, a recent posting on the Association of American of Physicians and Surgeons provides us with some interesting data that should give us and our political overlords cause to ponder their actions. Please note that all of the data presented in this posting is linked from the original sources on the AAPS webpage.
Here is a screen capture showing the lead in for the article:
The article opens by noting the following information about the size of SARS-CoV-2 particles, giving us a sense of just how small they are:
The article goes on to note the following:
"1.) Virus is transmitted through respiratory droplets produced when an infected person coughs, sneezes or talks. Larger respiratory droplets (>5 μm) remain in the air for only a short time and travel only short distances, generally <1 meter. They fall to the ground quickly. This idea guides the CDC’s advice to maintain at least a 6-foot distance.
2.) Virus-laden small (<5 μm) aerosolized droplets can remain in the air for at least 3 hours and travel long distances."
The curator of the article, Dr. Marilyn M. Singleton goes to to state that ventilation, even the opening of a door or small window, can dilute the concentration of droplets to one-half their original concentration after 30 seconds. This factor is critical given the issues facing users of poorly ventilated and highly populated areas like mass transit and long-term care facilities and why social distancing may not work as well as in other settings.
Dr. Singleton notes that a person can contract COVID-19 from touching surfaces and then touching their own mouth, nose and possibly eyes, however, it is not believed that this is the main source of viral spread.
Now, let's look at her research regarding masks. Here is some background on masks and respirators, remembering that the SARS-CoV-2 virus is 0.125 µmeters in size:
1.) Masks and respirators work by collecting particles through several physical mechanisms, including diffusion (small particles) and interception and impaction (large particles)
2.) N95 filtering facepiece respirators (FFRs) are constructed from electret (a dielectric material that has a quasi-permanent electric charge. An electret generates internal and external electric fields so the filter material has electrostatic attraction for additional collection of all particle sizes. As flow increases, particles will be collected less efficiently. A properly fitted N95 will block 95% of tiny air particles down to 0.3 μm from reaching the wearer’s face. But even these have problems: many have exhalation valve for easier breathing and less moisture inside the mask.
3.) Surgical masks are designed to protect patients from a surgeon’s respiratory droplets, aren’t effective at blocking particles smaller than 100 μm.
Here are the filter efficiencies of a number of materials that are used for filtering as follows:
Filter efficiency was measured across a wide range of small particle sizes (0.02 to 1 µm) at 33 and 99 L/min.
1.) N95 respirators had efficiencies greater than 95% (as expected).
2.) T-shirts had 10% efficiency,
3.) Scarves 10% to 20%,
4.) Cloth masks 10% to 30%,
5.) Sweatshirts 20% to 40%, and
6.) Towels 40%.
All of the cloth masks and materials had near zero efficiency at 0.3 µm, a particle size that easily penetrates into the lungs.
Another study which evaluated 44 masks, respirators and other materials with similar methods and small aerosols (0.08 µm and 0.22 µm) young the N95 FFR filter efficiency was greater than 95 percent, medical masks were 55 percent efficient, general masks were 38 percent efficient and handkerchiefs were between 2 percent effective (one layer) and 13 percent effective (4 layers).
The conclusions are as follows:
1.) Wearing masks will not reduce SARS-CoV-2.
2.) N95 masks protect health care workers, but are not recommended for source control transmission.
3.) Surgical masks are better than cloth but not very efficient at preventing emissions from infected patients.
4.) Cloth masks will be ineffective at preventing SARS-CoV-2 transmission, whether worn as source control or as personal protective equipment (PPE).
Masks may confuse that message and give people a false sense of security. If masks had been the solution in Asia (where masks are very commonly used for all respiratory infections), shouldn’t they have stopped the pandemic before it spread elsewhere?
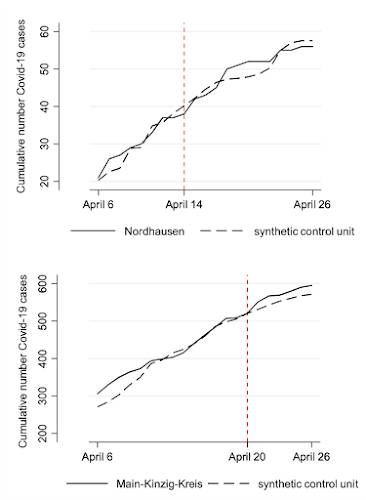
I want to close this posting with a graphic from Swiss Policy Research. The graphs show the cumulative number of COVID-19 infections against time and the date when mandatory masks were introduced with a vertical dashed red line for two German districts:
As you can see, there was very little negative impact on the rise in infections when mandatory mask wearing was introduced.
It is becoming increasingly apparent that a significant number of governments around the world from city to state/province to country are imposing masks on their citizenry without really considering the significant divisions in the medical community regarding their use. It is a rare government that takes a stand against the commonly held perception that masks perform as a cure all for stopping the spread of the COVID-19 pandemic.
Click HERE to read more from this author.
You can publish this article on your website as long as you provide a link back to this page.


Be the first to comment