A recent paper that appeared on the World Health Organization's website provides us with clear insight into the Infection Fatality Rate or IFR from research conducted by one of the world's leading epidemiologists, Dr. John P.A. Ioannidis, Professor of Medicine at the Stanford.
Let's start by looking at Dr. Ioannidis' background:
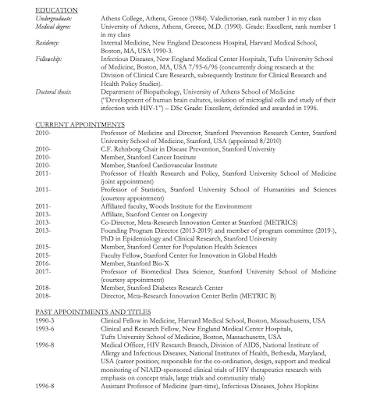
Here is a screen capture from his CV showing his education, current appointments and past appointments and titles:
Between 1994 and 2019, Dr. Ioannidis has published 1026 peer-reviewed studies (single author in 145 articles and first author in 302 articles) in some of the world's leading medical journals and is considered one of the most cited medical scientists in the world.
Now, to ensure that we are all on the same page, here are two key definitions:
1.) Infection fatality rate or IFR – is calculated by dividing the number of deaths by the number of actual infections with a given virus (i.e. individuals that have antibodies to the virus from seroprevalence tests meaning that asymptomatic individuals are included)
2.) Case fatality rate or CFR – is calculated by dividing the number of deaths by the number of confirmed cases of the disease (i.e. those individuals that exhibit clinical symptoms of the disease, hence, excluding asymptomatic individuals).
According to the aforementioned article that provided the definitions for both IFR and CFR, understanding the true infection fatality rate has major implications for planning control measures, particularly in the era of the SARS-CoV-2 pandemic.
With that background, let's now look at Dr. Ioannidis' contribution to the world's understanding of the infection fatality rate of COVID-19 as it appears in this peer-reviewed paper on the World Health Organization's own website:
While in the deluge of news that has been broadcast since the SARS-CoV-2 virus began to kill Chinese citizens living in Wuhan, we may have forgotten the original fear that was created by the world's media. At that time, early data from China suggested that there was a 3.4 percent case fatality rate and, given that asymptomatic infections were uncommon, the case fatality rate and the infection fatality rate would be the same.
For the purposes of his research, Dr. Ioannidis used data from 82 eligible seroprevalence studies which are defined as the overall occurrence of a disease within a defined population as measured using blood tests or, in other words, the frequency of individuals in a population with antibodies to a particular disease, in this case, COVID-19. The author used studies that had at least 500 assessed samples to eliminate issues with large uncertainty which would be introduced by smaller data sets. He included studies that had made seroprevalence assessments at different time intervals as well as long as there were at least 500 participants. For consistency, he used the entire population (all ages) and separately the population from 0 to 70 years of age to estimate numbers of infected persons, assuming that the seroprevalence would be similar in different age groups but recorded any significant differences in seroprevalcned across all age strata to determine the validity of his assumption. For the number of COVID-19 deaths, he chose the number of deaths accumulated until the date one week after the midpoint of the study period which accounts for delays in developing antibodies versus dying from infection. He does note that because of imperfect diagnostic documentation, COVID-19 deaths may have been both undercounted and overcounted in different locations at different points in time. With this data, he caudated the inferred infection fatality rate (IFR) by dividing the number of deaths by the number of infected people for the entire population and separately for people less than 70 years of age.
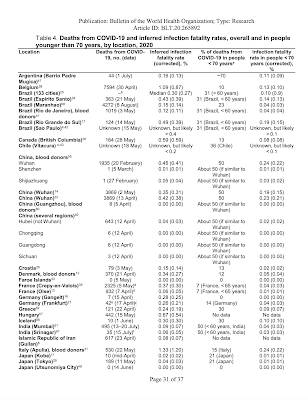
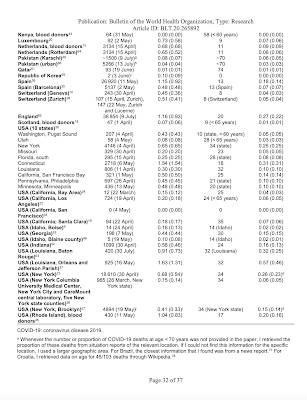
Dr. Ioannidis notes that he utilized 82 studies that were either published in peer-review literature or preprints up to September 9, 2020 with 24 studies using random sampling of the population, a much more robust method of determining the infection fatality rate. He also notes that several of the studies concentrated on geographical locations with high numbers of deaths, a factor that would result in a higher infection fatality rate on average. Here is a table showing the inferred infection fatality rate estimates for the studies used in Dr. Ioannidis' analysis:
Here is a summary of the results of Dr. Ioannidis' study:
"Infection fatality rates ranged from 0.00% to 1.63%, corrected values from 0.00% to 1.54%. Across 51 locations, the median COVID-19 infection fatality rate was 0.27% (corrected 0.23%): the rate was 0.09% in locations with COVID-19 population mortality rates less than the global average (< 118 deaths/million), 0.20% in locations with 118–500 COVID-19 deaths/million people and 0.57% in locations with > 500 COVID-19 deaths/million people. In people < 70 years, infection fatality rates ranged from 0.00% to 0.31% with crude and corrected medians of 0.05%.
The infection fatality rate of COVID-19 can vary substantially across different locations and this may reflect differences in population age structure and case- mix of infected and deceased patients and other factors. The inferred infection fatality rates tended to be much lower than estimates made earlier in the pandemic."
In general, the mortality rate for seasonal influenza is usually below 0.1 percent according to the World Health Organization as shown here:
"For seasonal influenza, mortality is usually well below 0.1%. However, mortality is to a large extent determined by access to and quality of health care."
Here is the author's final conclusion:
"…based on the currently available data, one may project that over half a billion people have been infected as of 12 September, 2020, far more than the approximately 29 million documented laboratory-confirmed cases. Most locations probably have an infection fatality rate less than 0.20% and with appropriate, precise non-pharmacological measures that selectively try to protect high-risk vulnerable populations and settings, the infection fatality rate may be brought even lower."
As well, as the use of serological testing continues to grow, the number of asymptomatic individuals that test positive for SARS-CoV-2 antibodies will also rise at the same time as the number of COVID-19 deaths has levelled off or fallen, resulting in a dropping infection fatality rate,
In any case, Dr. Ioannidis' research clearly shows that the all-age mortality of the SARS-CoV-2 virus is far lower than was originally estimated in early 2020 and is currently only roughly twice that of seasonal influenza and even significantly lower than that among people younger than 70 years of age, a fact that you are unlikely to hear in the mainstream media since it doesn't follow their narrative of COVID-19 fear-mongering.
Click HERE to read more from this author.
You can publish this article on your website as long as you provide a link back to this page.




Be the first to comment