A recent study by researchers at the University of Toronto and other institutions provides us with a clear picture of the effectiveness of the current COVID-19 vaccines against both the Omicron and Delta variants of the SARS-CoV-2 virus.
Here is a page showing the authors of the study and their affiliations:
The object of the study was to estimate vaccine effectiveness or VE against infections caused by both Delta and Omicron variants.
The authors looked at data from the Province of Ontario in Canada (Canada's most populous province) and estimated the effectiveness of the vaccine against infection irrespective of symptoms and severity caused by the Delta and Omicron variants between November 22 the day when the first case of Omicron was identified in Ontario and December 19, 2021. Individuals with at least 2 COVID-19 vaccine doses with at least one dose being an mRNA vaccine were included and the effectiveness over time of the two or three doses was estimated using multivariable logistic regression which establishes the relationship between a dependent variable (the outcome of interest) and more than one independent variable. At the time of the study, 88 percent of Ontarians aged 12 and older had received two doses of COVID-19 vaccine. Long-term care residents were excluded from the study as were individuals who had received only 1 dose of COVID-19 vaccine or who had received their second dose 7 days or less prior to being tested as well as individuals who had received two doses of the AstraZeneca or Johnson& Johnson vaccines. It is also important to note that Ontario began to roll out its third dose (i.e. booster) program in August 2021 primarily to residents of long-term care and retirement homes with individuals 70 years and older qualifying on November 6 followed by individuals aged 50 years and older on December 13 and individuals aged 18 and older on December 18.
The final data base used by the researchers included 9,201 Delta positive cases and 3,442 Omicron positive cases with Omicron cases being more common among younger males (mean age of 34.9 years compared to 45.0 years) and were less likely to have comorbidities.
After 2 doses of COVID-19 vaccines (with at least one being an mRNA vaccine), the vaccine effectiveness against the Delta variant waned as follows:
84% – 7 to 59 days after second dose
71% – greater than or equal to 240 days after second dose
After the third dose, the vaccine effectiveness rose to 93 percent 7 days or longer after receiving an mRNA vaccine.
After two doses of COVID-19 vaccines, the vaccine effectiveness against the Omicron variant was as follows:
38 percent – 120 to 179 days after the second dose
42 percent – 180 to 239 days after the second dose
After the third dose, the vaccine effectiveness against Omicron was only 37 percent 7 days or longer after receiving an mRNA vaccine.
This finding is similar to the findings of a study in Denmark where the vaccine effectiveness against Omicron was only 55.2 percent in the first 30 days after receiving a third dose and waned quickly.
In closing, here is the authors' conclusion:
"Two doses of COVID-19 vaccines are unlikely to protect against Omicron infection. While VE against Omicron infection is substantially lower than against Delta infection, a third dose of mRNA vaccine affords some level of protection against Omicron infection in the immediate term. However, the duration of this protection and effectiveness against severe disease are uncertain. Additional tools beyond the currently available vaccines, such as public health measures, antivirals, and updated vaccines, are likely needed to protect against Omicron infection."
Let's take a brief detour and look at a press announcement from Pfizer dated December 8, 2021 with the pertinent sections highlighted:
While Pfizer touts that a third dose of its COVID-19 vaccine may provide "more robust protection" against Omicron using its current vaccine, it is still hoping to roll out a variant-specific version of the vaccine designed for Omicron by March 2022. As an aside, you will also note that Pfizer's Chairman and Chief Public Officer Albert Bourla claims that "ensuring as many people as possible are fully vaccinated with the first two dose series and a booster remains the best course of action to prevent the spread of COVID-19" even though it hasn't so far. He forgot to mention that the three dose course is guaranteed to improve Pfizer's profitability.
We have to question why governments are pushing so hard to get their "subjects" to accept a third dose of the same vaccines that have been less than a stellar success over the short- to medium-term when studies are showing that these vaccines do not appear to be terribly effective against the Omicron variant even when initially administered, a factor that has led to Pfizer "tweaking" the current formulation of its BNT162b2 vaccine?
That said, remember that this "war" was never about a virus.
Addendum:
In the December 31, 2021 edition of the United Kingdom's Health Security Agency's Technical Briefing which looks at the vaccine effectiveness for Omicron (among other issues) we find this fascinating graph:
Notice how the effectiveness of Pfizer's BNT162b2, the gold standard of COVID-19 vaccines, against Omicron wanes very quickly, starting at just under 70 percent reaching roughly 50 percent within ten weeks of a third dose. Does this mean that a fourth (or fifth) dose will be necessary and that governments will continue to push the third dose mantra in spite of the data?
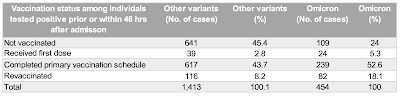
While some of my readers will say that the third dose will prevent or reduce hospitalizations, recent data from Denmark dated January 3, 2021 shows the following:
Only 24 percent of hospitalizations of Omicron-infected patients were unvaccinated compared to 52.6 percent who were fully vaccinated (under the old definition of two doses) and 18.1 percent were triple vaccinated, roughly the same percentage as those who remain unvaccinated give or take 6 percentage points.
I remain open to any explanations that my readers may offer to explain this data.
You can publish this article on your website as long as you provide a link back to this page.




Be the first to comment