Back in early April 2021, this "Rapid Response" appeared on the website of the British Medical Journal (BMJ):
Should you happen to look at the URL of the article, you will note that it appears on the Archive.is webpage capturing website. It also appears on the Wayback Machine Thankfully, the internet never forgets anything.
Should you happen to go search for the original article as it appeared on the BNJ website, this is what you'll find:
The original "Rapid Response" was written by Dr. Katya Polyakova-Nelson, the Medical Director of Partnerships in Care, Kent as shown here:
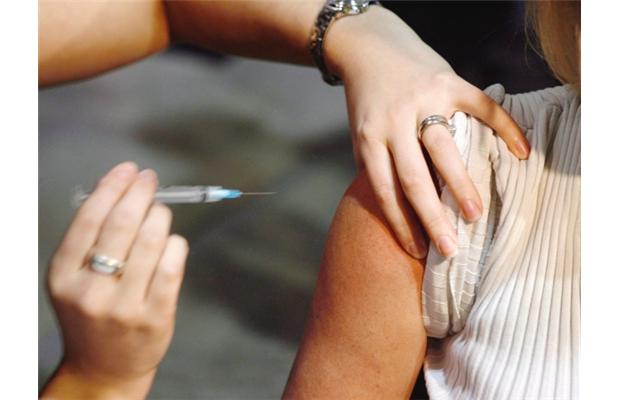
…who was writing a letter to the Editor of The BMJ in response to this article entitled "Do doctors have to have the covid-19 vaccine?" published on March 29 2021:
In the original article, four medical professionals weigh in on whether doctors should be required to be injected with the COVID-19 vaccines as part of a program to reduce risks to their patients. Here is a brief look at what each "expert" advised:
1.) Vageesh Jain, public health specialty registrar, University College London:
"As it stands, legally, you don’t have to have a covid vaccine. But ethically, clinically, epidemiologically—whichever way you slice it—I would argue you do.
The ethical case is grounded in the professional duty healthcare workers have to protect their patients: do no harm. Although everyone has the right to decide whether to take a vaccine or not, patients (often elderly or unwell, and therefore vulnerable to covid-19) also have fundamental rights to be protected from avoidable harm. When these principles come into conflict, actions that safeguard the best interests of patients must be favoured.
The evidence on covid-19 vaccines is clear: they are safe and they work. Some are understandably concerned about a lack of long term data, but the importance of this can be overstated. For other vaccines, mild side effects can occur in the first few months but serious and longer term problems are largely theoretical for most."
2.) Colin Melville, General Medical Council medical director and director of education and standard:
“It’s been an incredibly challenging year with many uncertainties and difficult decisions about patient care, alongside concerns about our own wellbeing and the wellbeing of those around us. The arrival of covid-19 vaccines provides new tools to protect patients, doctors, and their families, and with the progress of the rollout we are, hopefully, starting to see a light at the end of the tunnel.
Most, if not all, doctors should now have been offered one of the vaccines. And, for most, the benefits are clear. But some may be hesitant, and we’ve received queries from doctors asking what our guidance says about being vaccinated.
“Our advice, set out in our guidance on the professional standards expected of all doctors, says, ‘doctors should be immunised against common serious communicable diseases, unless this is contraindicated.’
“So, while there is no absolute duty to be vaccinated, you must consider the risk of spreading coronavirus to patients, particularly those who are clinically vulnerable."
3.) Rob Hendry, medical director at the Medical Protection Society: –
"While the vaccination is recommended, it’s not currently mandatory and there are no contractual obligations, so healthcare workers cannot be forced to have it.
They should, however, be mindful of the GMC’s Good Medical Practice, which states that ‘doctors should be immunised against common serious communicable diseases, unless this is contraindicated.’ Its covid-19 guidance also states that ‘there is a potential risk of inadvertently spreading coronavirus to vulnerable patients. This weighs in favour of doctors being vaccinated unless there are good reasons why it isn’t appropriate in your individual circumstances.’
Medical staff who refuse the vaccine should therefore be prepared to justify their decision and, where possible, mitigate any risks. We would encourage healthcare workers who are reluctant or refuse the vaccine to explore their increased risk of repeated exposure to the virus, the benefits of the vaccination to colleagues, patients, and family, and the wider benefits of reducing the transmission of covid-19 with their supervisor and occupational health."
4.) Sarah Ali, consultant in diabetes and endocrinology, Royal Free London NHS Foundation Trust:
“Working as a patient facing doctor and looking after people who are considered to be clinically vulnerable meant that taking the vaccine was an easy decision for me.
Based on the premise that vaccines are effective at reducing the transmission of covid-19, I saw it as protecting not only myself but also the community, especially those at high risk of morbidity and mortality from covid-19 and those who are unable to have the vaccine.
Additionally, I consider the vaccine to be our strongest tool to exit the pandemic in a timely manner, and minimise the significant economic, societal, and psychological impact the pandemic is continuing to have."
You will note that in all four cases the experts claim that the vaccines will prevent transmission of the virus to patients. This is interesting given that the vaccine manufacturers clearly stated that the ability of their COVID-19 vaccines to prevent the transmission of the SARS-CoV-2 vaccine is an unknown quantity. In one case, the expert even describes the possibility of long-term side effects and serious adverse reactions as "theoretical" which is interesting given that Phase 3 trials are not scheduled to end until 2022 – 2023.
Let's take a brief look at the key paragraphs in Dr. Katya Polyakova's response which has been censored by the BMJ which shows the downside of the vaccines and their side effects with bolds being mine:
"...what I am currently struggling with is the failure to report the reality of the morbidity caused by our current vaccination program within the health service and staff population. The levels of sickness after vaccination is unprecedented and staff are getting very sick and some with neurological symptoms which is having a huge impact on the health service function. Even the young and healthy are off for days, some for weeks, and some requiring medical treatment. Whole teams are being taken out as they went to get vaccinated together.
Mandatory vaccination in this instance is stupid, unethical and irresponsible when it comes to protecting our staff and public health. We are in the voluntary phase of vaccination, and encouraging staff to take an unlicensed product that is impacting on their immediate health, and I have direct experience of staff contracting Covid AFTER vaccination and probably transmitting it. In fact, it is clearly stated that these vaccine products do not offer immunity or stop transmission. In which case why are we doing it? There is no longitudinal safety data (a couple of months of trial data at best) available and these products are only under emergency licensing. What is to say that there are no longitudinal adverse effects that we may face that may put the entire health sector at risk?
What has happened to “my body my choice?” What has happened to scientific and open debate? If I don’t prescribe an antibiotic to a patient who doesn’t need it as they are healthy, am I anti-antibiotics? Or an antibiotic-denier? Is it not time that people truly thought about what is happening to us and where all of this is taking us?
The cancel culture is alive and well during the age of COVID-19 and is, apparently, thriving in the global medical community.
You can publish this article on your website as long as you provide a link back to this page.

Be the first to comment